My current project is to document – through ink-and-wash paintings – some backyard wild birds I have seen over the past years. Birdwatching, like art, is quite therapeutic, I’ve found. Like art it requires patience and good observation skills, and it requires you to be in the moment. I’m barely a hobbyist and I’ve certainly not committed to buying professional photography equipment, so I do the best I can taking photos with my phone. You can see some of my photos below:
Due to equipment limitations, the birds in the photos are all at a distance and thus no good for reference, so I have to pull images from the internet to serve as my guide when I paint. Below is a peek at one of the pieces in progress, inked but not painted yet. Can you guess what bird it is?

I’ve been feeling very awkward with my paints and pens and brushes – a symptom of having done very little artwork for so long, no doubt, and also I’m not feeling entirely like myself while under therapy.
These bird paintings, therefore, serve more as a warm-up and refresher. At least, I’m staying productive. And I’m definitely glad something beautiful can come out of this otherwise distressing time. I’ll be ready to share more of the artwork next week, so do come back for that. Chemo doesn’t seem so bad as long as I get to paint and draw.
Speaking of which, I did mention last time that I would share more about the Chemo experience. So for those of you who are maybe heading into chemo, or know someone who will be, or if you are just curious, let me tell you what chemotherapy looks like for me:
But First, My Chemo Bag
Minus a few items that I left out that are very personal to me, here’s everything I bring to a chemo session:
- Lab results – printed or digital copy, but already forwarded to my doctor as well, so she can advise me if any of the results are concerning
- Prescriptions – digital copy. Sometimes the doctors need a reminder of the meds they prescribed.
- Phone stand – so I can sit back in my recliner without having to hold the phone
- Phone charger and/or power bank
- Earphones – so I don’t disturb the other patients while watching or listening to stuff
- Sketchbook – to sketch, in case I feel up for it. For my mental therapy.
- Pencil case with pens, pencils, eraser – the necessary tools, of course.
- Breakfast and coffee – I take my breakfast at the hospital. Since my treatment is about 6 hours long, I leave the house before sunrise to beat the traffic and get ahead of other patients so I can also finish early in the afternoon.
- Lunch – you get very hungry and very thirsty
- Socks – I’m barefoot in my step-ins, but once at the hospital I take my shoes off and my feet will get cold because of the airconditioning so I come prepared. It’s also partly for hygiene reasons, gloves on my feet.
- Pillow – would bring one, but I always forget. The head rest on the recliner is too high for me and hits the top of my head not the nape, so it’s uncomfortable to sit/lie back comfortably. A pillow would help.
- Jacket – It gets cold. Fair warning, if your jacket is on as the IV line is inserted, the jacket stays on until the end of the session.
- Tissue
- Alcohol
- Extra Mask
- Mints – for after meals and in case I feel nauseated
- Snack – As I mentioned, I get hungry…
- Water – … and thirsty
- Laptop – it seemed like a good idea the first time, but I just end up doing stuff on the phone.
- Laptop charger
- Wallet – usual wallet stuff
- PWD ID – digital copy. My physical. ID is still pending release.
- Important documents – you don’t need all your medical records, but bring the most recent labs, and anything relevant to insurance, or welfare, etc. Digital copies are usually enough.
The Chemotherapy Session
For me, it’s 6 cycles of Chemo using the drugs paclitaxel and carboplatin. Each cycle is made up of 2 sessions, one week apart, followed by a rest week. So 3 weeks to a cycle.
On the day of a session, for around 6 hours, I sit in a recliner that fits within a small cubicle. There are other patients in identical, adjoining cubicles and in a row across from me as well.
It begins with a quick vitals check by one of the nurses (hardworking underpaid nurses, I might add). The Oncology fellow then comes and asks me some questions: am I feeling ok, did I take my meds, any mouth sores, vomiting, etc. If my lab results are within the acceptable limits, I’m cleared for today’s chemo session. I then wait for the pharmacist to prepare my chemo meds. The nurse then comes and prepares the Intravenous (IV) line and then inserts the IV catheter, usually in one of the veins on the back of my hand. Once the IV line is inserted you’re pretty much “strapped in” until the meds are all done. To use the bathroom, one must press a call button and have the nurse assist you to hold and transfer the fluid bottle and line when you make your way to the toilet. The nurse waits outside the bathroom, in case you were wondering, unless of course you need the assistance.
So, IV line in, pre-meds done and then the chemo drugs. Now, you can just sit back and relax… unless you have a reaction to the medicines, which I did at one point:
It was during my third session that I first experienced it. I was just about to doze off when I felt a slight pressure in my chest, which quickly turned into a more palpable tightness – almost as if someone were squeezing my heart and lungs. I felt my face get flushed and my breathing become difficult. Getting scared, I hit my call button then called out to the nurse that was attending to the patient in the cubicle across from me. She turned, gasped when she saw what I assume was my red face and distressed breathing: “Ay, you’re having a reaction!” She immediately jumped into action. Other nurses and the onco fellow came and gathered around me. Someone injected hydrocortisone into my IV line. I tried very hard not to panic and sat quietly, concentrating on breathing in and out even though it was difficult to do so. The doctor checked my heart with her stethoscope, somebody else attached a blood pressure monitor around my arm. Slowly my breathing started to normalize. I got a bit emotional and may have cried a few quiet tears.
I reacted to the chemo drugs in two more succeeding sessions, but each time the reaction became milder because I’d been pre-medicated with higher doses of steroids and the chemo meds were titrated and given more slowly.
Things have been going smoothly at each session since then and I actually kind of look forward to my quiet time sitting in my favorite cubicle where I can be alone with my thoughts because, well, you don’t really have any other choice.
Of course, Netflix and other online distractions are available at your fingertips if you have your phone with you (which I do) and you access the hospital WIFI or use your mobile data. Sometimes, I’ll catch up on some of my favorite series or watch a movie. Mostly I will either sleep – because the diphenhydramine makes me drowsy – or I’ll write or draw.
It’s also nice to chat with your fellow patients and the nurses. And it’s probably the most real life social interactions that I’ve had with people since the pandemic started. But do take into account that I’m highly introverted and never really chose to socialize much even before Covid.
Except for the reaction to the drugs, if you go in with a positive mindset, and maybe a plan to somehow be productive, even if that just means that you commit to getting your rest, the chemo session can be not just endurable but also restful.
It’s after the chemo session that’s really the tough part, and I’m not talking about the hairloss.
After The Session
It’s the first week of November as I write this. If all goes well, my treatment, which began in mid-August, should be done by the first week of December.
I cannot say enough how art and staying productive is a big help. Walking my dogs is also good for keeping me moderately exercised, which helps with some of the side effects. So, if going into chemo, exercise and, I would encourage you to find something creative that you’ve always wanted to try (that’s not too physically taxing) and do it during your time in therapy.
Of course, I have down days when the most I can do is lie down and move about only as needed. It starts around the next day or sometimes two days after my treatment. My tummy feels bloated, but I also feel hungry at the same time. And yet, I can’t eat because the food tastes off and it’s difficult to swallow. And when I don’t eat I, of course, start to feel weak.
There are some foods I can eat but just barely. Nuts are great, almonds especially. Fruits, yes. Muesli bars, unsalted biscuits and crackers, too. Sweet things mostly still taste sweet, so I also have Honey coated corn flakes in whole milk, oatmeal sweetened with condensed milk and champorado (chocolate porridge) on standby. Sweet stuff in moderation though, I would caution. When the off taste starts to fade – usually by the third day post-treatment, I can transition to more savory meals with Lucky Me Pancit Canton Calamansi flavor, and Fita crackers with some spinach dip or cheese spreads. Not entirely healthy stuff, I know, but I recall at least one medical expert advising that you should just eat what you can eat at this point. Of course, individual preferences will vary.
And, Of Course, Hairloss.
The first thing you should know is that it will grow back. Hairloss doesn’t happen for all types of chemo, but it does for mine.
I was kind of excited about it at first, imagining how it would be a chance for me to try some wigs, play around with styles, reinvent my look. But then the hair actually starts to fall out and things start to get real.
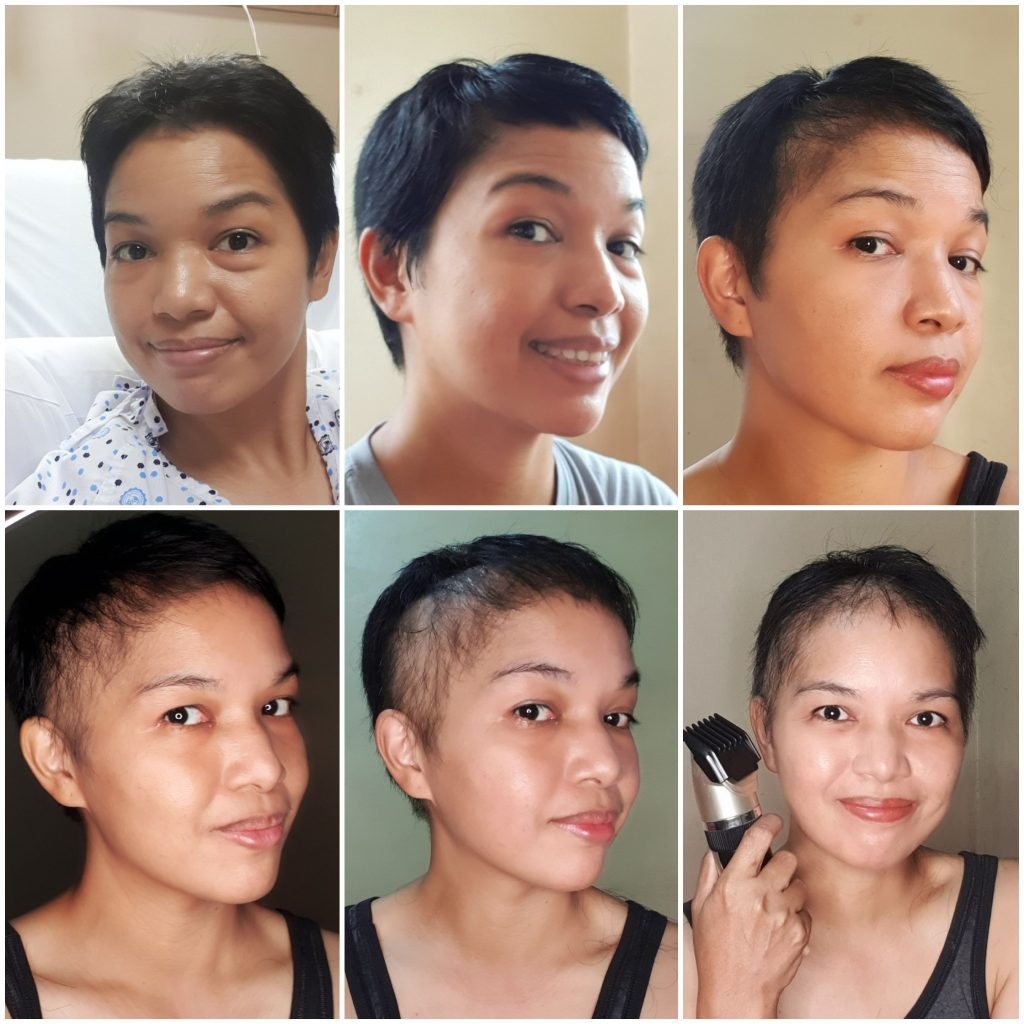
It started at about 3 sessions in. Having short hair to begin with made it a lot less messy, but it still got messy. One day, you wake up and notice the hairs accumulating on your pillow, then when you brush or shampoo more and more of it comes out. A few strands at a time at first, and then in clumps. It was mildly distressing, but it helped to be aware and prepared for what was to come.
I sat in front of the mirror every day, racking up the courage to get ahead of the hairfall, be done with it and just shave it all off so I wouldn’t have to deal with picking up after myself all the time. My friend Shirley described me perfectly – I was basically a perpetually shedding labrador. By the time I was brave enough to run a clipper over my scalp, most of the hair was gone anyway so shaving the rest off wasn’t really a big deal.

It was a relief to be done with that transitional phase. I don’t think bald works for me though, so to make myself feel better, I had a little photo shoot to try my temporary going-out look (see photos below). I must say a big thank you to my friend Owen who some years ago had her own bout with cancer and chemo and who sent me some of her beanies in preparation for going bald.
And that’s how you’ll see me these days, with a beanie or a cap and a little hairpiece for bangs to give the illusion of a full head of hair. A wig, I find, is intolerably hot if you wear it outside of air-cooled conditions.
My eyebrows started to go after Cycle 4, so now I have to draw them in with an eyebrow pencil. The plus side of the hairloss is that I don’t have to shave in many other parts mentionable and unmentionable and I’ll leave that to your imagination.
So that’s life with chemo.
And here’s where I’ll end yet another lengthy blog post, and thank you once again for indulging if you made it this far.
As I mentioned, if you’re headed into chemo, please feel welcome to reach out to me and ask questions. You can email me at hello@marosemagpily.com.
I hope I’ll find you here again next week. I’ll get back to sharing more about my artwork, such as it currently is. I think what I need is to get back to the basics and just get reacquainted with the different media, build up my confidence again and paint and draw without expectations. But more on that next time.
Take care and be well until then!